Ankylosing spondylitis (AS) can be difficult to diagnose.
That’s because the symptoms can mimic those of other conditions.
Back pain is extremely prevalent in the modern world which is why ankylosing spondylitis often goes undiagnosed, or misdiagnosed, for years or even decades.
When a patient comes in with a set of AS symptoms it’s dismissed as back pain.
The advice is to get a better office chair… see a physiotherapist… exercise more.
While all of this good advice (and helpful for everyone, whether they have AS or not) it does not address the root cause.
The good news is that there are several tests that doctors can use to diagnose ankylosing spondylitis.
First, they’ll ask you about your medical history and symptoms.
Typically questions are:
“When did your symptoms start?”
“What makes them worse?”
“What makes them better?”
They’ll ask if there is any family history of AS (as in at least 90% of cases there is a genetic component).
Next, the doctor will perform a physical exam.
They’re looking for signs of inflammation, such as swelling in the joints and they will also look at your posture and flexibility.
That’s because AS can cause physical changes to the spine which affects how you stand or move.
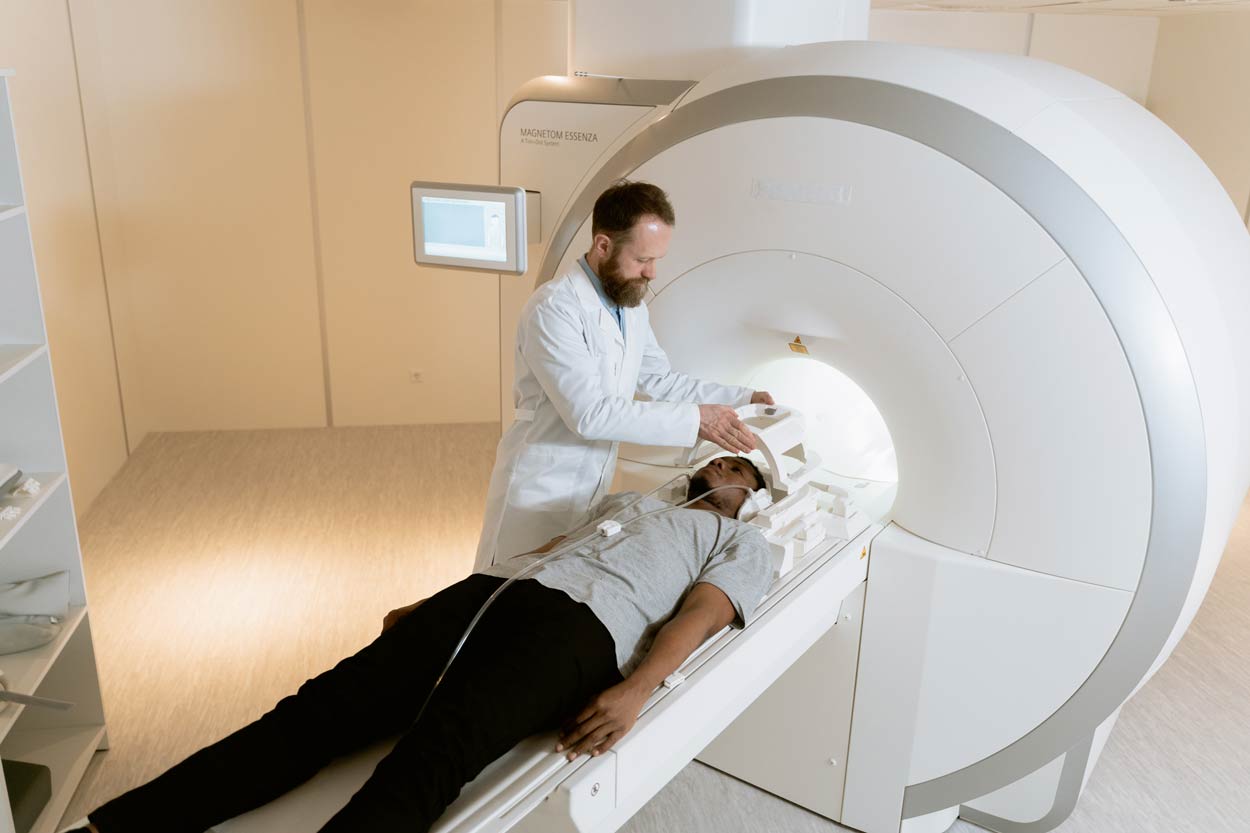
If the they suspect you may have AS, they can then order imaging tests such as X-rays or magnetic resonance imaging scans (MRI scans).
X-rays can show changes in the joints and bones, such as fusion of the spine or erosion of the joints.
MRI scans can pick more nuance and show inflammation in the joints and soft tissues, such as the tendons and ligaments.
As well as the imaging tests, your doctor can order blood tests to check for markers of inflammation.
Typically they will look at C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR). If these levels are high it indicates that the body is fighting something which is further evidence of AS, potentially.
They will also test for the HLA-B27 gene. This is the genetic marker most commonly associated with a higher risk of developing AS (and is found in over 90% of patients).
If there is some indication that the patient may have AS they will likely refer them to a rheumatologist.
Rheumatologist specialise in diagnosing and treating arthritic conditions such as ankylosing spondylitis.
They’ll then review the your medical history, perform a physical exam, and order any additional tests (i.e. anything you haven’t had yet) to confirm the diagnosis.
Early diagnosis is so important for managing AS, so if you think you may have it please get in touch with your doctor.
This was a quick 2 minute explainer. For my more detailed guide on AS diagnosis, click here:



0 Comments